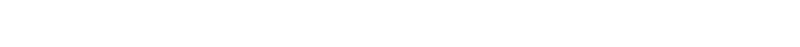From treatment delays for victims of rural traffic crashes to a dwindling number of rural hospitals delivering babies, the State Journal's yearlong series, "Out of Reach: The Rural Health Care Gap," has chronicled many rural health care challenges — and solutions. As the series ends with this installment, here's a quick look at some of the problems and efforts to address them:
Staffing shortages: A shortage of primary care doctors and specialists, such as obstetricians and child psychiatrists, is especially severe in rural areas.
Possible solutions
•Midlevel providers — chiefly, physician assistants and nurse practitioners - are filling in, though in some rural places they are also in short supply. Midwives and new types of workers, including community paramedics and dental therapists, also help fill the gap.
People are also reading…
•The Wisconsin Academy for Rural Medicine, UW School of Medicine and Public Health's new training track for rural doctors, should make physicians more available in small towns. The state's second pharmacy school, which opened this fall at Concordia University in Mequon, could produce more rural pharmacists. There's also talk of a second dental school, in Marshfield.
•Payments to offset school debt increased under the new federal health care law to $170,000 for doctors and other providers who work in underserved areas for five years. Wisconsin offers up to $100,000 to doctors for a three-year commitment to certain rural areas.
Distance: The geographic isolation and sparse population density that define many rural areas give medical providers little financial incentive to provide services.
Possible solutions
•Telemedicine allows rural patients to see doctors in larger cites through video connections for a variety of services, including pain management, psychiatry, pharmacy and emergency treatment for strokes.
•Machines can sometimes deliver services without providers present, such as InstyMeds booths that dispense drugs in some rural places where pharmacies have closed.
•Electronic medical records should allow rural hospitals and clinics to communicate better with urban facilities, though the records are a financial strain.
Socioeconomics: Rural Americans are more likely to be poor and, in most states, uninsured. Groups such as the Amish have special health care needs.
Possible solutions
•Free clinics in rural Wisconsin and free programs in other states, such as Kentucky Homeplace and Remote Area Medical, treat or assist people who can't pay or are uninsured. The Wisconsin Dental Association's annual Mission of Mercy event offers free dental care.
•Grassroots initiatives address specific needs, such as the Iowa-based Seeds of Hope's mental health hot line for farmers in Wisconsin and the Riverway Communities of Hope, a nonprofit in Blue River that pays for substance abuse and mental health counseling for teenagers.
•In Lancaster, midwives and a doctor have opened a farmhouse for births, mostly for Amish families who prefer not to deliver in hospitals.
Money: Payments from the government health plans Medicare and Medicaid are too low to support certain rural services, such as dental care and nursing home care, providers say.
Possible solutions
•Federally qualified health centers are expanding dental care for low-income people in many places, including Cashton, Darlington and Dodgeville. The new federal health care law gives the health centers more money.
•The Wisconsin Dental Association has proposed Medicaid rate increases for dentists - unlikely given the state's budget shortfall. But teeth cleanings by dental hygienists in schools are expanding.
•A study in Montana could lead to frontier hospital networks, which would get a new kind of government payment to help sustain nursing homes and other services in remote areas, including in Wisconsin.