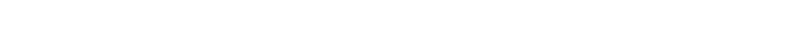Northwest Indiana cardiologists are implanting the latest in pacemaker technology. And they say patients are reaping the benefits.
"The recovery is a lot quicker. There's no scarring. It's done through a puncture in the leg. The risk of infection is a lot less than the conventional way," said Dr. William Espar, an interventional cardiologist with Franciscan Health hospital in Michigan City.
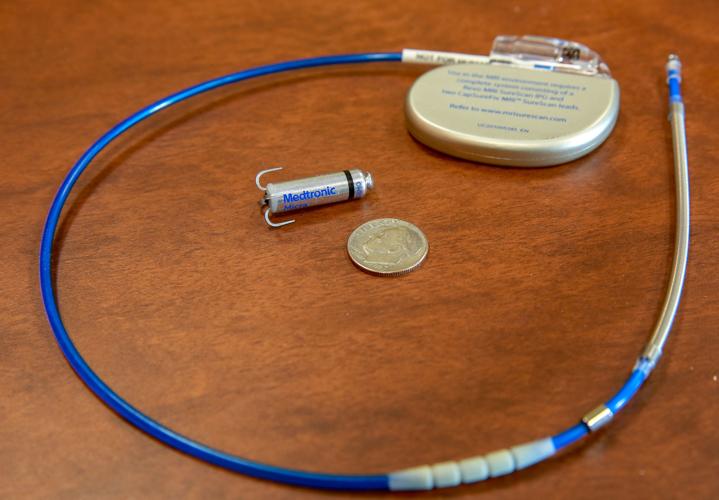
He said the new leadless pacemakers are about the size of a vitamin — 10 times smaller than a traditional pacemaker. In November, he implanted the first one at his hospital, in an 81-year-old Michigan City woman.
Region heart specialists have been putting in dozens of the Medtronic Micra pacemakers over the past year and a half, which were approved by the Food and Drug Administration in 2016 and Medicare in 2017. As of now, the devices are only an option for patients who need pacing in the bottom chamber of the heart.
People are also reading…
Local heart experts say the leadless pacemakers are good for cardiac patients with the rhythm disorder atrial fibrillation, or who have comorbidities, especially those who require chemotherapy, immunosuppression or dialysis and thus are at risk of infection. About a quarter of patients qualify.
Traditional pacemakers, used for decades, had wires called leads screwed into the heart that would stay in the bloodstream and deliver electrodes to the organ.
"Like any electrical cable, if they wiggle enough they break — especially with a 100,000-times-a-day beating heart," said Dr. Samer Ajam, an electrophysiologist with Community Healthcare System, whose Munster Community Hospital was the first in the Region to implant a Micra.
So the leads would have to be replaced a lot. The devices also were more prone to infection from the bloodstream, in which case the whole system would have to be changed out.
The new pacemakers, Ajam said, are "completely injected inside the heart, completely encapsulated; they kind of get absorbed into the heart tissue itself."
"The less hardware you put into somebody's body, the less chance of getting infected," he said.
He noted, however, that the new pacemakers have about the same battery life — eight to 10 years — as traditional ones. He recommends replacing a traditional pacemaker with the leadless kind only if the former breaks or the patient develops a condition in which an infection would be life-threatening.
Loretta Pierce, a 78-year-old Valparaiso retiree, had one of the devices implanted by Ajam in December 2017. Her heart problems stretch to the mid-1990s, when she had four bypasses. She later had eight stents put in her heart. But her condition kept worsening.
Diagnosed with atrial fibrillation, she tried medication and a heart monitor. Nothing worked. Then her heart rate dropped to 30 beats per minute, well below the normal range. Still, she was reluctant to get a pacemaker.
Then, one night, she said, "My heart felt like it was stopping. I felt like, 'I'm going to die, anyway. I'll go ahead and take the pacemaker then.' "
Ajam told her about the Micra, which she said is "no bigger than .22 bullet." She thought, "The newer technology the better — but you don't want to be the guinea pig, either."
The doctor assured her it was safe. She got it put in and has been doing well ever since, she said.
"I go grocery shopping, do some of my housework. I take my own baths, get dressed. I have a lot more energy," she said.
"Would I do it again? In a heartbeat."
After the procedure, patients go home the next or even same day, said Dr. Sandeep Sehgal, an interventional cardiologist at Porter Regional Hospital in Valparaiso. He noted that traditional pacemakers had to be implanted through the patients' chest wall.
"They don't have anything sticking out in the chest now," he said. "Normally, older patients are smaller and have this big bulge in their chest, which is uncomfortable, and they have pain from the scarring."
Region heart specialists predict the smaller, leadless pacemakers will become the norm in the next few years, once a device that protects both the atriums and ventricles is developed, perhaps one that uses Bluetooth technology for the chambers to communicate. And those physicians — Methodist Hospitals also does the new pacemakers — plan to offer it locally.
Sehgal said that unless patients need a heart transplant or pump, they don't have to leave the Region for cardiac care.
"Short of cardiac transplants, Northwest Indiana is up to speed with all the devices and everything," he said.