Computer scientists at Stanford have created a deep learning algorithm to visually diagnose skin cancer that matched the performance of board-certified dermatologists, Stanford News reports. According to a recent paper published in the Jan. 25 issue of Nature, the final product based on a database of nearly 130,000 skin disease images was tested against 21 board-certified dermatologists and successfully matched the performance of the dermatologists in diagnosing the most common and deadliest skin cancers.
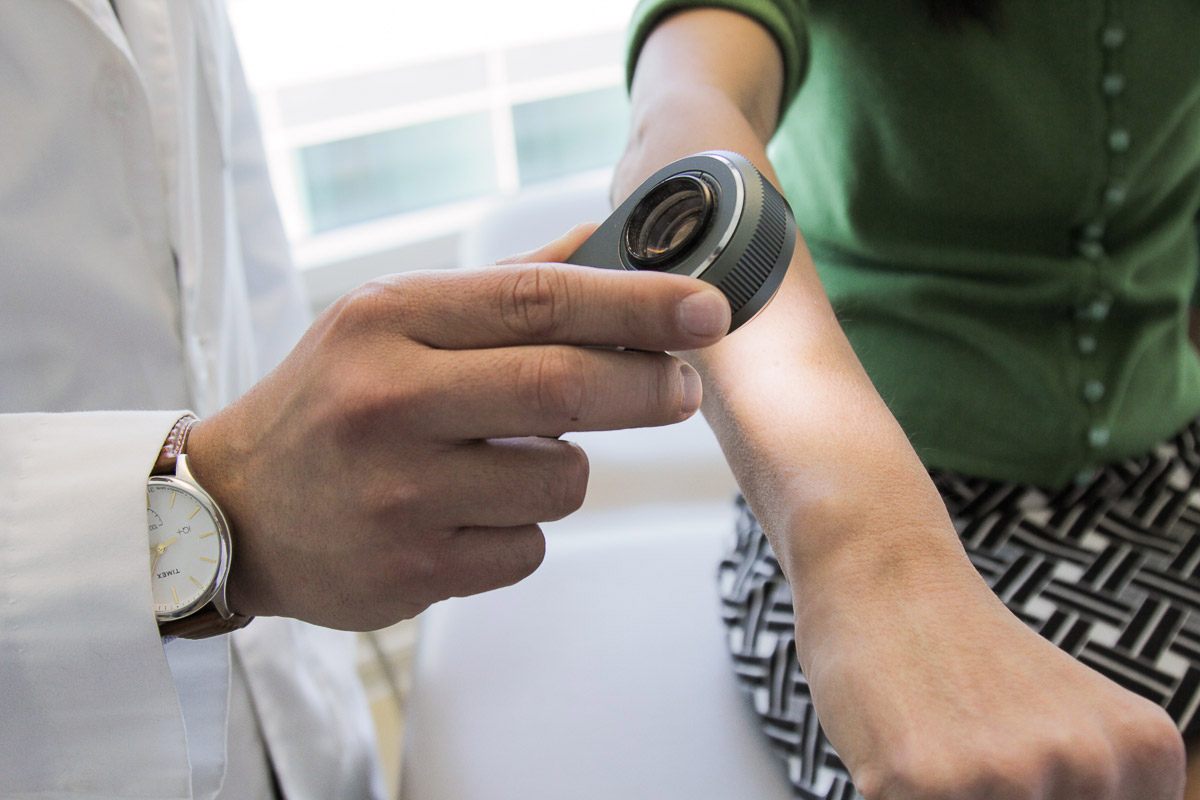
Each year, there are more than 5.4 million new cases of skin cancer in the United States. Early detection is critical to skin cancer outcomes with five-year survival rate for melanoma detected in its earliest states is around 97 percent; however, if left undetected the rates drops to 14 percent. Diagnosing skin cancer typically with a visual examination usually looking at the suspicious lesion with the naked eye and with the aid of a handheld dermatoscop. For patients with limited access to healthcare, an option to receive a diagnosis via a smartphone could be life saving.
“We made a very powerful machine learning algorithm that learns from data,” said Andre Esteva, co-lead author of the paper and a graduate student in the Thrun lab. “Instead of writing into computer code exactly what to look for, you let the algorithm figure it out.”
To build the algorithm, Stanford researchers started with an algorithm developed by Google that was already trained to identify 1.28 million images from 1,000 object categories. The researchers then collaborated with dermatologists to identify each image as raw pixels with an associated disease label allowing the algorithm to work off a wider variety of data. After going through the necessary translations, they collected about 130,000 images of skin lesions representing over 2,000 different diseases.
To test the algorithm, researchers used only high-quality, biopsy-confirmed images provided by the University of Edinburgh and the International Skin Imaging Collaboration. 21 dermatologists were asked whether, based on each image, they would proceed with biopsy or treatment, or reassure the patient. Success of the product was evaluated based on how well the dermatologists were able to correctly diagnose both cancerous and non-cancerous lesions in over 370 images.
“There’s no huge dataset of skin cancer that we can just train our algorithms on, so we had to make our own,” said Brett Kuprel, co-lead author of the paper and a graduate student in the Thrun lab. “We gathered images from the internet and worked with the medical school to create a nice taxonomy out of data that was very messy – the labels alone were in several languages, including German, Arabic and Latin.”
The algorithm’s performance criteria was measured sensitivity-specificity curve, where sensitivity represented its ability to correctly identify malignant lesions and specificity represented its ability to correctly identify benign lesions. The sensitivity-specificity curve was assessed through through three key diagnostic tasks:
1. Keratinocyte carcinoma classification
2. Keratinocyte carcinoma classification
3. Melanoma classification when viewed using dermoscopy
In all three tasks, the algorithm matched the performance of the dermatologists with the area under the sensitivity-specificity curve amounting to at least 91 percent of the total area of the graph. In the future, the team would like the implement the algorithm on a mobile device; however, the it still needs further testing in a real-world clinical setting.
“Advances in computer-aided classification of benign versus malignant skin lesions could greatly assist dermatologists in improved diagnosis for challenging lesions and provide better management options for patients,” said Susan Swetter, professor of dermatology and director of the Pigmented Lesion and Melanoma Program at the Stanford Cancer Institute, and co-author of the paper. “However, rigorous prospective validation of the algorithm is necessary before it can be implemented in clinical practice, by practitioners and patients alike.”
Image credit: Matt Young
